Measurement and Monitoring of Safety Framework
The release of the Measurement and Monitoring Safety Framework (MMSF) in 2013 catalyzed a major change in the way safety is defined and practiced and has informed and influenced Heathcare Excellence Canada’s approach. Created by Professor Charles Vincent and colleagues at The Health Foundation, the MMSF proposed shifting away from focusing on the absence of harm towards adopting a broader view of safety. This new view examined the sources of resilience and capabilities that enable safe care and endorsed a less reactive approach to improving safety.
The MMSF offers many advantages when it comes to how we think about safety. It:
- creates a more holistic view of safety.
- changes our safety focus – moving away from a focus on past harm.
- provides a shared and consistent understanding of safety.
- changes the way we think about safety.
- helps us move away from managing risk to managing safety.
- moves us from assurance and accountability reporting to a "practice of inquiry."
- empowers everyone to take a proactive role in safety.
- promotes a culture of collective responsibility for safety.
- promotes an understanding that staff and patient safety go hand in hand.
- places value on soft intelligence (e.g. listening, observing and perceiving).
- recognizes the value that patients and caregivers have in creating safety.
How it works
MMSF is made up of five dimensions that healthcare leaders, providers, patients and families can use to understand and improve patient safety. The framework assesses and evaluates safety from "ward to board" by providing a comprehensive and accurate real-time view of patient safety. It helps users move from "assurance" to "inquiry" by shifting away from a focus on past cases of harm towards current performance, future risks and organizational resiliency.
"The framework for the Measurement and Monitoring of Safety helps people rethink their understanding of safety in their own clinical environment," says Dr. Baker. "What we saw during the demonstration project is that staff were really engaged by this idea that they can have an active role in promoting and maintaining safety."
- Dr. G. Ross Baker, PhD, Professor, Institute of Health Policy Management and Evaluation, University of Toronto
Armed with a series of valuable questions, you can make better decisions about the safety of the care you provide. The primary questions are:
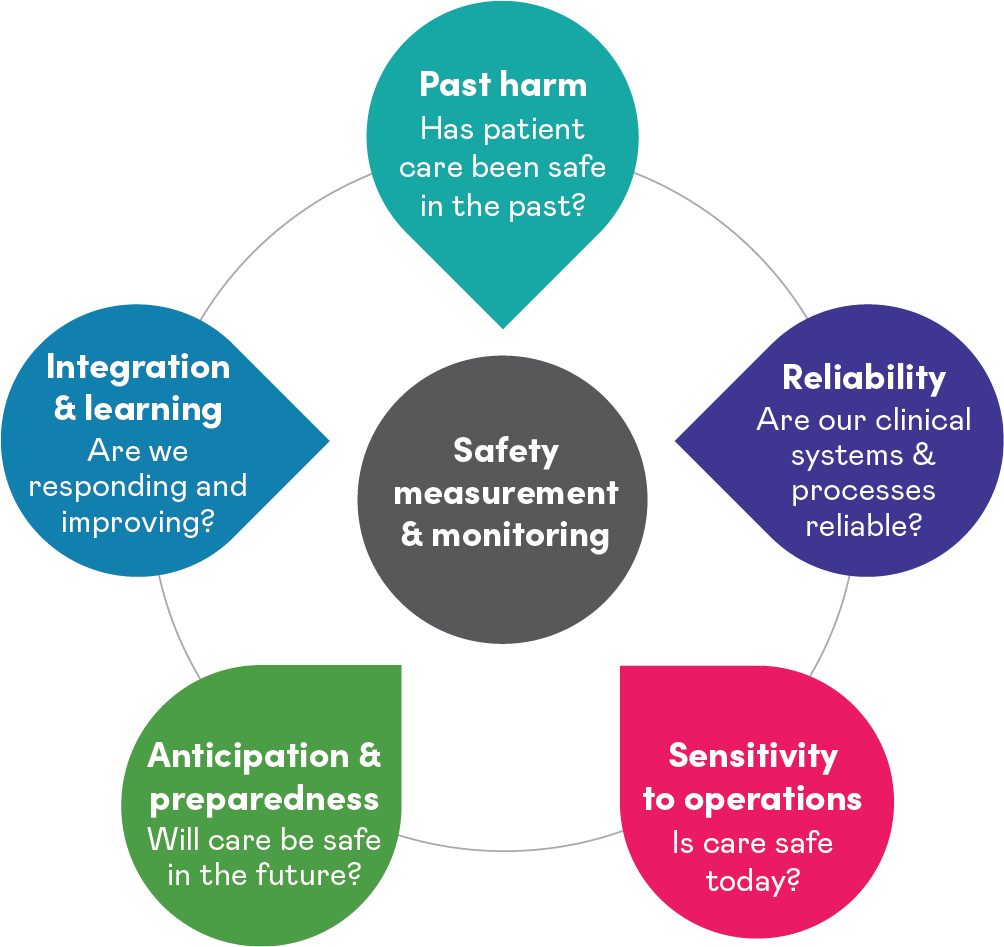
Applying the framework in Canada
In 2017, the Canadian Patient Safety Institute (which amalgamated with the Canadian Foundation for Healthcare Improvement to form Healthcare Excellence Canada in 2021), began working with healthcare teams from across the country to advance our knowledge and experience of the MMSF in Canada. Following a successful demonstration project led by Dr. G. Ross Baker at the University of Toronto, a subsequent learning collaborative was launched in 2018 with 11 teams from seven provinces. With expert faculty and mentoring over 18 months, each team used the MMSF to develop a more comprehensive approach to delivering safer care.
An evaluation in 2020 concluded that the collaborative successfully built the capacity of teams to understand and implement the MMSF in their local settings. Participants reported positive impacts on stakeholder groups' knowledge and behaviours, healthcare processes and patient outcomes.
"We started out in the safety world really worrying about past harm and I think that was really important because it raised peoples' understanding about the magnitude of the safety issues. But it is insufficient because people don't go to work thinking about past incidents; they go to work thinking about the patients they are going to see today. So that is part of the shift now is that we are putting safety into a much more relevant context for the staff on their units doing their daily jobs. I think we can still build on that. We can build a broader sense of how units function, and how units interact with other units."
- Dr. G. Ross Baker, PhD, Professor, Institute of Health Policy Management and Evaluation, University of Toronto
Learn more:
- Measurement and Monitoring of Safety Framework: a qualitative study of implementation through a Canadian learning collaborative | BMJ Quality & Safety
- Measurement and Monitoring of Safety Framework (MMSF): learning from its implementation in Canada | BMJ Quality & Safety
Measuring and monitoring safety: A patient and care partner perspective
The evaluation showed that the MMSF improved safety practices and was well-received by frontline teams, senior leaders and board members. Limited attention, however, had been paid to how patients engage with this wider view of safety.
The release of How Safe is Your Care? Measurement and monitoring of safety through the eyes of patients and their care partners provides important insights into how patients and their care partners see safety. The report offers guidance on how to effectively engage patients and care partners in all aspects of measurement and monitoring of safety and provides recommendations outlining how to strengthen provider and patient partnerships in support of safer care.
Learn more: